The Way Forward: High-Dose, Short-Course Levofloxacin Leads the Field
Question 9
How important are atypical pathogens in the etiology of CAP?
| In recent years, the prevalence of atypical pathogens in CAP has been reported to be higher than previously recognized, possibly driven by greater efforts to identify causative pathogens in the development of new antibiotics. This may also be due to improved techniques for identification of the atypical pathogens. Historically if a “typical pathogen” was identified, the search ended. In many clinical trials identification measures for atypicals have been initiated at the start of therapy with the frequent finding of diagnostic evidence of multiple pathogens frequently both typical and atypical, even as high as 40% in some series (51, 52). In most reports the incidence of Chlamydia pneumoniae ranges from 5.0% to 27.2%, M. pneumoniae 1.1% to 25.9% and Legionella pneumophila 3.9% to 10.5%. The role of atypicals is also seen to increase when infections caused by more than one pathogen are considered (Figure 4). Because identification of causative pathogens is rarely available at the time of diagnosis, antibacterial coverage for atypical bacteria is recommended in all major guidelines by the pulmonary and infectious disease experts when initiating empiric treatment for CAP. It should be mentioned, however, that many of these earlier incidence studies used serology to identify atypicals, and the infectious disease community has now moved from diagnosis based on a single high diagnostic titer, to one requiring a 4-fold change in titer or identification through culture or polymerase chain reaction (PCR). Therefore, the incidence of atypicals in early studies may be overstated in some cases. It is currently not established whether co-pathogenecity versus sequential infection, as is known to occur in influenza outbreaks, may be invoked. |
Figure 4. Incidence of typical and atypical pathogens and co-infection rates among CAP patients
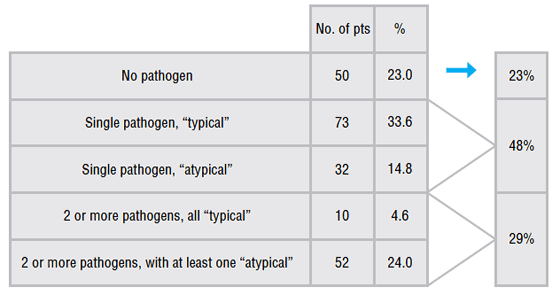
Abbreviations: CAP = community-acquired pneumonia, pts = patients.
Adapted from reference (53).










