The Way Forward: High-Dose, Short-Course Levofloxacin Leads the Field
Question 19
Could you comment on the problem of resistance and how should this problem be managed?
As we are aware the incidence of resistance, particularly among respiratory tract pathogens, continues to grow (Figure 6). While the development of new antimicrobial agents is an essential component in the effort to remain ahead of emerging microbial resistance this has to be coupled with judicious use of current antimicrobials in order to maintain their efficacy. Unrestrained use of these agents will predictably lead to further expansion of resistance. A more sensible strategy is to identify new ways to use current drugs to increase the duration of their usefulness. This includes methods to optimize antibiotic selection, dose, and duration of therapy. The World Health Organization (WHO) recommends using the most potent agent for the shortest amount of time to limit the risk of resistance development.
Evidence is accumulating that the application of policies that optimize antibiotic selection, dose, and duration of therapy can reduce or reverse the emergence of resistant pathogens without compromising patient care (70, 71). Therefore, in order to reduce resistance it is important to use knowledge of the PK/PD parameters of agents to maximize not only their efficacy but also their ability to be less likely to select for resistance.
Figure 6. TRUST studies 2005-2007: antimicrobial resistance of Streptococcus pneumoniae in the United States
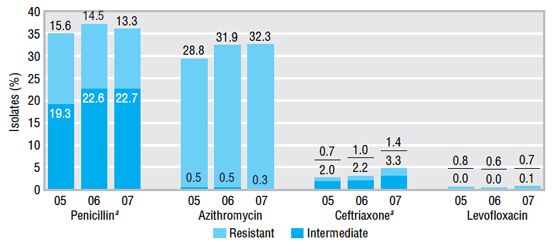
In vitro activity does not necessarily correlate with clinical results.
2005 = 4,958 isolates, 184 labs; 2006 = 3,932 isolates, 157 labs; 2007 = 3,720 isolates, 163 labs.
a Penicillin (oral) and ceftriaxone (non-meningitis).
Adapted from reference (68, 69).









