Levofloxacin for extended-spectrum beta-lactamase- (ESBL-) producing Enterobacteriaceae infections
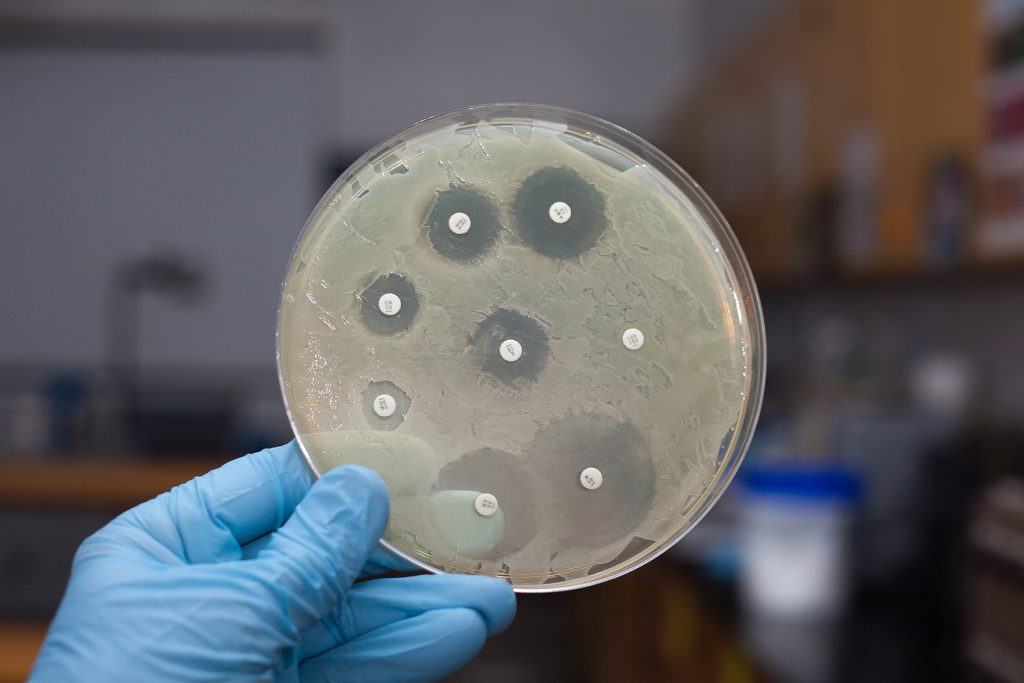
Levofloxacin is shown to be a treatment of choice for hospitalised patients with extended-spectrum beta-lactamase- (ESBL-) producing Enterobacteriaceae infections.
ESBL is an enzyme that confers resistance to most beta-lactam antibiotics, including penicillin, cephalosporins, and aztreonam.1 Increasing resistance to standard carbapenem therapy has been reported in ESBL-producing Enterobacteriaceae infections; although limited evidence is available, the use of cefepime, fluoroquinolone, and piperacillin/tazobactam is shown to be effective.1
Investigators at the Texas Tech University Health Sciences Center performed a retrospective chart review at a 522-bed (including 22 intensive care units) community hospital; records of patients receiving cefepime, levofloxacin, or carbapenem between 1 January 2012 and 30 September 2015 were included. The study aimed to evaluate clinical outcomes of these three antimicrobials commonly used as alternative treatment for ESBL-producing Enterobacteriaceae infections in rural healthcare institutions.
The predominant infections treated among patients (n=113) were urinary tract infections, skin and soft tissue infections, and intra-abdominal infections.1 There were no statistically significant differences in hospital mortality – the primary outcome of the study – in all three antimicrobial groups. However, the investigators found an association between carbapenem treatment and an increased risk of mortality; and a reduced risk of mortality with cefepime or levofloxacin treatment.1 The ICU length of stay and hospital length of stay were shorter in both the cefepime and levofloxacin groups compared to the carbapenem group.
While previous studies had demonstrated improved inpatient mortality with ciprofloxacin and levofloxacin treatment – the primary type of infection was limited to bacteraemia.2-4 The current study provided better insights into the clinical outcomes of the alternative treatments for different sources of infection as well as multiple Enterobacteriaceae spp including Escherichia coli, Klebsiella pneumoniae, and Proteus mirabilis. In addition, cefepime dosing had been adjusted for therapeutic efficacy in this study – considering the association between low-dose regimens and increased mortality.5
The investigators thus recommend the use of cefepime and levofloxacin as potential alternative antimicrobials for the treatment of infections with ESBL-producing Enterobacteriaceae isolates that are susceptible. Further studies with larger cohort are warranted.
Source
Clinical outcomes of extended-spectrum beta-lactamase-producing Enterobacteriaceae infections with susceptibilities among levofloxacin, cefepime, and carbapenems.
PMID: 29670677
DOI: 10.1155/2018/3747521
Link: https://www.ncbi.nlm.nih.gov/pubmed/29670677
References
- Walker KJ, et al. Can J Infect Dis Med Microbiol 2018;2018:3747521.
- Defife R, et al. Antimicrob Agents Chemother 2009;53:1074-1079.
- Lo C, et al. J Microbiol Immunol Infect 2015;50:355-361.
- Drago L, et al. J Antimicrob Chemother 2001;48:37-45.
- Andreatos N, et al. Open Forum Infect Dis 2017;4:ofx113.










