Optimizing the Management of Prostatitis: Levofloxacin and Silodosin—Strategies Aimed at Optimal Treatment for Prostatitis
Optimal Antimicrobial Therapy for Prostatitis


Optimal management of acute bacterial prostatitis begins with empiric parenteral fluoroquinolones or β-lactams before switching to oral administration, with adjustments made according to susceptibility testing. Oral therapy is then usually continued for 2 to 4 weeks.
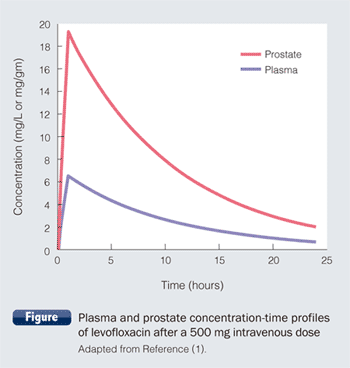
The management of chronic bacterial prostatitis is much more problematic, with a wide range of both Gram-positive and -negative pathogens responsible for the disease, making it essential that antibiotic therapy provides a wide range of coverage. This has led to the fluoroquinolones becoming the drugs of choice for treating chronic bacterial prostatitis as they possess broad-spectrum activity against both traditional and atypical uropathogens. In addition, they have favorable pharmacokinetics with a high distribution into prostatic tissue. The fluoroquinolone levofloxacin is particularly effective in treating urinary tract infections (UTIs) and bacterial prostatitis as it exhibits high renal excretion and excellent penetration into prostatic and urinary sites. This is highlighted by 500 mg levofloxacin achieving a plasma concentration of > 6 mg/L which increases more than 3-fold to almost 20 mg/L in the prostate (Figure)(1).
 |
| Click on image to enlarge. |
In contrast, the β-lactam, doripenem, has a much lower penetration into prostatic tissue (2). Of even greater relevance for successful therapy of chronic bacterial prostatitis is the good penetration achieved by levofloxacin into prostatic fluid, as this has been shown to be associated with even greater clinical efficacy (3). It is also well known that the urinary excretion rate of levofloxacin is very high at 84%, compared with much lower values for ciprofloxacin (43%) and moxifloxacin (20%) (4) providing levofloxacin with advantageous pharmacokinetic and pharmacodynamic (PK/PD) features compared with other fluoroquinolones.
High-dose levofloxacin (750 mg) has also been shown to achieve higher plasma concentrations than the 500 mg dose, with a 1.9-fold increase in the maximum concentration (Cmax) and a 2.3-fold increase in the area under the concentration-time curve (AUC0-24h). A clinical investigation of this confirmed that 750 mg levofloxacin given for 5 days was associated with a 91.3% clinical success in complicated UTIs and acute pyelonephritis compared with 88.4% for 10-day conventional ciprofloxacin therapy. In catheterized patients with a greater incidence of biofilm production, the 750 mg levofloxacin dose resulted even in a 78.9% eradication rate compared with 53.3% for ciprofloxacin. The 750 mg levofloxacin dose has also been shown to be well tolerated and safe. With fluoroquinolone resistance a concern, it is also important to note that levofloxacin achieves target pharmacodynamic ratios necessary to prevent the emergence of resistance in Pseudomonas aeruginosa (5).
In summary, while many antibacterials are not indicated for UTIs and prostatitis due to poor penetration into these sites, this is not the case for levofloxacin, which possesses advantageous PK/PD features enabling it to reach concentrations approximately 3 times higher in the prostate compared with plasma. This feature coupled with levofloxacin’s broad-spectrum pathogen coverage make it an excellent agent for treating these infections, with clinical efficacy confirmed in numerous studies (6).
References
(1) Drusano GL, et al. Antimicrob Agents Chemother 2000; 44: 2046-51.
(2) Yamada Y, et al. Int J Antimicrob Agents 2010; 35: 504-6.
(3) Bulitta JB, et al. Chemotherapy 2011; 57: 402-16.
(4) Naber KG. Int J Antimicrob Agents 2001; 17: 331-41.
(5) Karlowsky JA, et al. Clin Infect Dis 2005; 40 Suppl 2: S89-98.
(6) Naber KG, et al. Int J Antimicrob Agents 2008; 32: 145-53.









