The Treatment of Community-Acquired Pneumonia with Consideration of Mycobacterium Tuberculosis
Delay in the Tuberculosis Diagnosis Caused by Empirical Treatment of Community-Acquired Pneumonia


Evidence-based medicine has resulted in the development of guidelines that provide clear therapeutic strategies for clinicians treating CAP. Pre-eminent among these guidelines are those of IDSA and ATS, both of which recommend using respiratory fluoroquinolones in CAP in the presence of comorbidities or risk factors for drug-resistant S. pneumoniae. However, concern has grown regarding the potential delayed diagnosis and treatment of TB under this strategy. Dr. Jen-Jyh Lee, National Tuberculosis Association, Taiwan, reported results from a recent review clarifying this issue (1).
A comprehensive review and meta-analysis was performed to evaluate whether fluoroquinolones are associated with delayed treatment and increased resistance in TB. Nine studies were included in the final meta-analysis (4 focusing on delays in treatment and 5 on resistance) (Table 1).
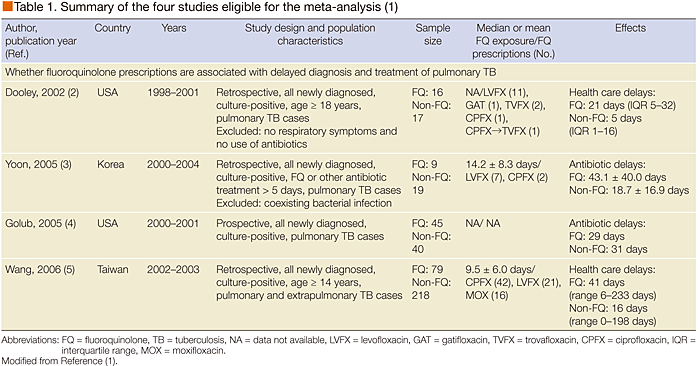
The first study confirmed that among patients receiving empiric fluoroquinolones, the median time between initial presentation and starting anti-TB therapy was 21 days compared with 5 days for those who did not receive fluoroquinolones (p = 0.04) (2). These results were supported by the second study, which revealed a longer delay in starting anti-TB medication in the fluoroquinolone group (43.1 ± 40.0 days vs. 18.7 ± 16.9 days, p = 0.04) (3). However, Dr. Lee noted the small sample size of both studies and that in the first study, only 3 of the 17 non-fluoroquinolone patients received no antibiotic, while the remaining 14 were treated with cephalosporins, macrolides, a combination of these, trimethoprim-sulfamethoxazole, or anti-TB therapy.
Interestingly, 83% of patients receiving fluoroquinolone monotherapy reported symptomatic improvement, and clinical improvement was documented 3 days after starting treatment. Dr. Lee stated that a clinical response to fluoroquinolones does not exclude the diagnosis of TB and, cannot be used to differentiate between CAP and TB. It is therefore necessary for clinicians to consider M. tuberculosis as a potential pathogen when a patient presents with CAP, and to initiate an appropriate diagnostic work-up.
The third study evaluated 158 subjects (85 received antibiotics prior to TB diagnosis, and 73 received TB therapy initially). There was a much greater delay in median health care for patients receiving antibiotics compared with those who did not receive antibiotics (39 days vs. 15 days, p < 0.01) (4). However, when looking specifically at antibiotic class, the median antibiotic delay for fluoroquinolones was 29 days compared with 31 days for other antibiotics, indicating that the delay was not due to the anti-TB activity of fluoroquinolones, but the time taken between initiation of therapy and waiting for a clinical response.
Dr. Lee then drew attention to the issue of chest X-ray analysis. In this study, only 57% of patients diagnosed with pneumonia had a chest X-ray and although 34% of these suggested a diagnosis of TB, empiric antibiotics were still initiated. He noted that both antibiotic use and not taking a chest X-ray at the first health care visit were independently associated with longer health care delays. The results from these studies led Dr. Lee to stress the need for physicians to comply with the IDSA and ATS guidelines for CAP and order chest X-rays before prescribing antibiotics. In addition, when the clinical examination or chest X-ray suggests TB, sputum examinations for acid-fast bacteria (AFB) should be ordered.
The fourth study investigated 548 patients with newly diagnosed culture-confirmed TB (79 received a fluoroquinolone, 218 received a non-fluoroquinolone antibiotic and 251 received no antibiotics before anti-TB treatment) (5). The median interval from the initial visit to starting anti-TB treatment was longer in the fluoroquinolone group (41 days) compared with both the other antibiotic group (16 days) and the no antibiotic group (7 days). Again, Dr. Lee drew attention to the fact that within a mean of 4 days of fluoroquinolone treatment, 65.8% of patients were found to exhibit clinical improvement, along with improved chest X-ray findings and laboratory data. It was also noted that although demographic characteristics between the fluoroquinolone and the other antibiotic groups were similar, those in the non-fluoroquinolone group who died tended to die earlier than in the fluoroquinolone group, possibly due to the anti-TB efficacy of the fluoroquinolone delaying disease progression.
Dr. Lee concluded that clinicians must remain very suspicious regarding the possibility of TB, especially in TB endemic areas. This should be the case regardless of whether clinical improvement is noted after the use of a fluoroquinolone, and appropriate bacteriological and histopathological tests for TB should be performed as early as possible.
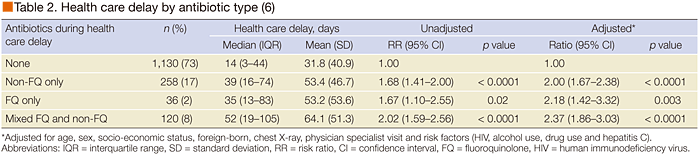
Another recent publication has added to this debate (6). Results from a population-based cohort of 2,232 patients with active TB evaluated 1,544 with full retrospective data. Of these 1,544 patients, 414 (27%) received antibiotics, while the remaining 1,130 (73%) did not. The average health care delay for patients exposed to antibiotics was significantly longer, with a median delay of 41 days in the antibiotic group compared with 14 days in the non-antibiotic group.
Stratification according to the type of antibiotic revealed that of the 27% of patients treated with prior antibiotics, 17% received non-fluoroquinolones, 2% received only fluoroquinolones, and 8% received combined therapy. There were no differences reported between those who received non-fluoroquinolone antibiotics, fluoroquinolones, and combined therapy in terms of a delay in TB diagnosis (Table 2). Therefore, the delay in starting anti-TB therapy is probably not related to the anti-TB effect of fluoroquinolones, but rather to the time required for taking the antibiotics and the subsequent waiting for a clinical response. Dr. Lee emphasized that these results support the view that previous treatment with any antibiotic, and not only a fluoroquinolone, is associated with a delay in TB diagnosis.
Finally, Dr. Lee summarized the results of a review investigating whether empirical treatment of CAP with fluoroquinolones not only delays treatment of TB, but also whether it results in greater M. tuberculosisresistance. He noted that the rate of fluoroquinolone-resistant TB was not related to previous brief fluoroquinolone exposure, but occurred more often with multidrug-resistant TB (MDR-TB), and recommended the use of fluoroquinolones in CAP patients with a shorter duration of disease (7). He concluded by noting that the International Standard for Tuberculosis Care, published in 2009, recommends that the diagnosis of sputum smear-negative pulmonary TB should be based on at least two negative sputum smears, a chest X-ray consistent with TB and a lack of response to a trial of broad-spectrum antimicrobial agents.
References
(1) Chen TC, et al. Int J Infect Dis 2011; 15(3): e211-6.
(2) Dooley KE, et al. Clin Infect Dis 2002; 34(12): 1607-12.
(3) Yoon YS, et al. Int J Tuberc Lung Dis 2005; 9(11): 1215-9.
(4) Golub JE, et al. Int J Tuberc Lung Dis 2005; 9(4): 392-7.
(5) Wang JY, et al. Thorax 2006; 61(10): 903-8.
(6) Wang M, et al. Int J Tuberc Lung Dis 2011; 15(8): 1062-8.
(7) Shen GH, et al. Int J Antimicrob Agents 2012; 39(3): 201-5.










